Research project
Lessons from the frontline: The impact of redeployment during Covid-19 on nurse well-being, engagement and retention
- Start date: 1 October 2020
- End date: 1 October 2021
- Partners and collaborators: University of Leeds, University of Oxford, Bradford Teaching Hospital Foundation Trust,
- Principal investigator: Professor Rebecca Lawton, University of Leeds
- Co-investigators: Professor Kerrie Unsworth, Leeds University Business School; Dr Michael Dunn, University of Oxford; Angela Grange, Bradford Teaching Hospital Foundation Trust; Dr Ruth Simms-Ellis, Bradford Teaching Hospital Foundation Trust.

Description
In February 2020 there were 335,171 nurses working in the NHS, approximately half of whom work in acute hospital care (NHS Digital). These nurses, working on the frontline during COVID-19 have experienced redeployment to specialties and teams they have never worked in before. They have struggled with inadequate or ill-fitting PPE and they have witnessed patients and relatives in distress. They have dealt with risk and uncertainty, huge changes to their ways of working over short periods of time and the constant worry for themselves and their family and friends that they may be transmitters of the disease.
This rapid readjustment was more keenly felt in areas where COVID-19 was most prevalent and in areas with high levels of the most vulnerable groups (older, poorer and more ethnically diverse populations). During the Covid-19 crisis staff redeployment has been extensive and varied. Some staff have been redeployed into high-risk areas from their relatively safe ‘home’ wards (Dunn et al, 2020).
Other staff who are at high risk or shielding have been moved off wards to different duties (personal communication). For example, in our local Trust (Bradford) staff in this category have been asked to provide telephone information and support (via the Electronic Patient Record) to relatives of patients who are in hospital but unable to receive visitors. These different forms of redeployment are likely to have different consequences, with the potential for trauma or moral injury in the first group and strong feelings of guilt in the second.
The emotional ramifications of working through Covid-19 are only beginning to be understood. For example, a recent survey by the Nursing Times found that over a third of nurses reported that their mental health was “bad” or “very bad” as a result of the COVID-19 pandemic (Nursing Times, 2020).
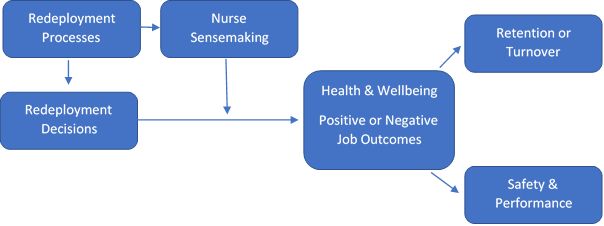
Our research programme, funded by National Institute of Health Research and headed up by Professor Rebecca Lawton, will examine how nurses were redeployed and how they adapted and coped with redeployment during Covid-19, as well as examining the effects on nurse well-being, engagement and retention.
The first work package, led by Dr Michael Dunn (University of Oxford) and Dr Angela Grange (Bradford Teaching Hospital Foundation Trust) will examine: How was the process of redeploying nursing staff managed prior to and during the Covid-19 crisis?
Method: Interviews with 30 senior staff (across 3 NHS Trusts) responsible for decision making about how, where and when staff were redeployed and what support was provided to these staff and how their return to previous teams was managed.
The second work package, led by Professor Kerrie Unsworth (University of Leeds) and Dr Ruth Simms-Ellis (Bradford Teaching Hospital Foundation Trust): What were the emotional and performative challenges for redeployed nurses and how did they adapt to and cope with their changing of roles during the Covid-19 crisis?
Method: Questionnaires and interviews with a sample of frontline staff at each Trust. We plan to recruit 60 staff in total (20 from each site) and follow them up at 3 points in time.


